Maternity Care
Are you expecting a baby?
At this uncertain time Lucie Seacroft, specialist midwife at Kingston Hospital explains the latest advice in pregnancy checks, nutrition, exercise and general wellbeing for expectant mothers
Lucie is one of the many experienced midwives working at Kingston Hospital, Surrey who has had the privilege of advising many parents-to-be what they should and shouldn’t be doing when it comes to eating habits, daily routines and emotional states.
Healthy diet
Staying healthy during pregnancy is paramount. Maintaining a healthy diet including vitamin supplementation and engaging in moderate exercise can benefit both you and your growing baby. Keeping healthy during this important time will also benefit you and your recovery once you have had your baby.
The Royal College of Obstetricians and Gynaecologists, which works to improve the health care for women across the world, advise women maintain a healthy diet prior to conception, during and after pregnancy. It suggests a varied diet including at least five portions of fruit and vegetables a day to ensure you get the right balance of nutrients you and your baby need. Although it’s always best to get the vitamins and minerals from the foods you eat, during pregnancy it is important for the development of your baby to also take a folic acid supplement. The NHS recommends that you take folic acid every day eight weeks prior to pregnancy and for up to 12 weeks into the pregnancy to reduce the risk of abnormalities e.g. spina bifida.
Vitamins
Additionally, it is advisable expectant mothers take a vitamin D supplement. Generally, we get enough vitamin D from the sunlight, however with reduced daylight hours during the winter months it is important not to let our levels of vitamin D intake decline. Vitamin D is essential in helping to regulate the amount of calcium and phosphate in our bodies, both of which are needed to help keep bones, teeth and muscles healthy. The dose you require of both folic acid and vitamin D may vary based on your body weight, so do ensure this is discussed and checked with your midwife or healthcare professional.

Eating for two?
You may be wondering whether being pregnant means that you need to “Eat for two”. The short answer is no. Although you may find yourself feeling more hungry than usual, which is very common, the current advice is not to increase the calories you consume. Instead, eat a low-fat daily diet and incorporate fibre-rich products (e.g. wholegrain varieties and brown rice); protein (e.g. salmon and pulses such as lentils, beans) and foods containing calcium (e.g. milk, cheese, yoghurt – although try to go for lower fat and lower sugar products where possible). When pregnant, it is also very important not to skip breakfast and to limit your caffeine intake to a maximum of 200mg per day, or even better, swap caffeinated drinks altogether with decaffeinated alternatives. It is also important to refrain from the use of alcohol and drugs. Currently, there is insufficient evidence to show what a safe level of alcohol is in pregnancy. We therefore recommend you do not drink any whilst pregnant.
Exercise
Lucie adds that women must listen to their body and adapt their activity accordingly. For example, intense running can be adapted to moderate jogging or walking. Women may notice that certain physical activity may feel different. Lucie’s advice is simple: “if the level of activity feels comfortable then continue. If it doesn’t feel comfortable, then stop and seek advice from your healthcare professional.” The key is to look after your bump so it is recommended that expectant mothers avoid contact sports and other activities that include a high risk of trauma or falling onto your abdomen. If you do ‘bump the bump’ the best advice is to try and not panic, but instead contact your health care professional for advice as soon as possible if you have any concerns.
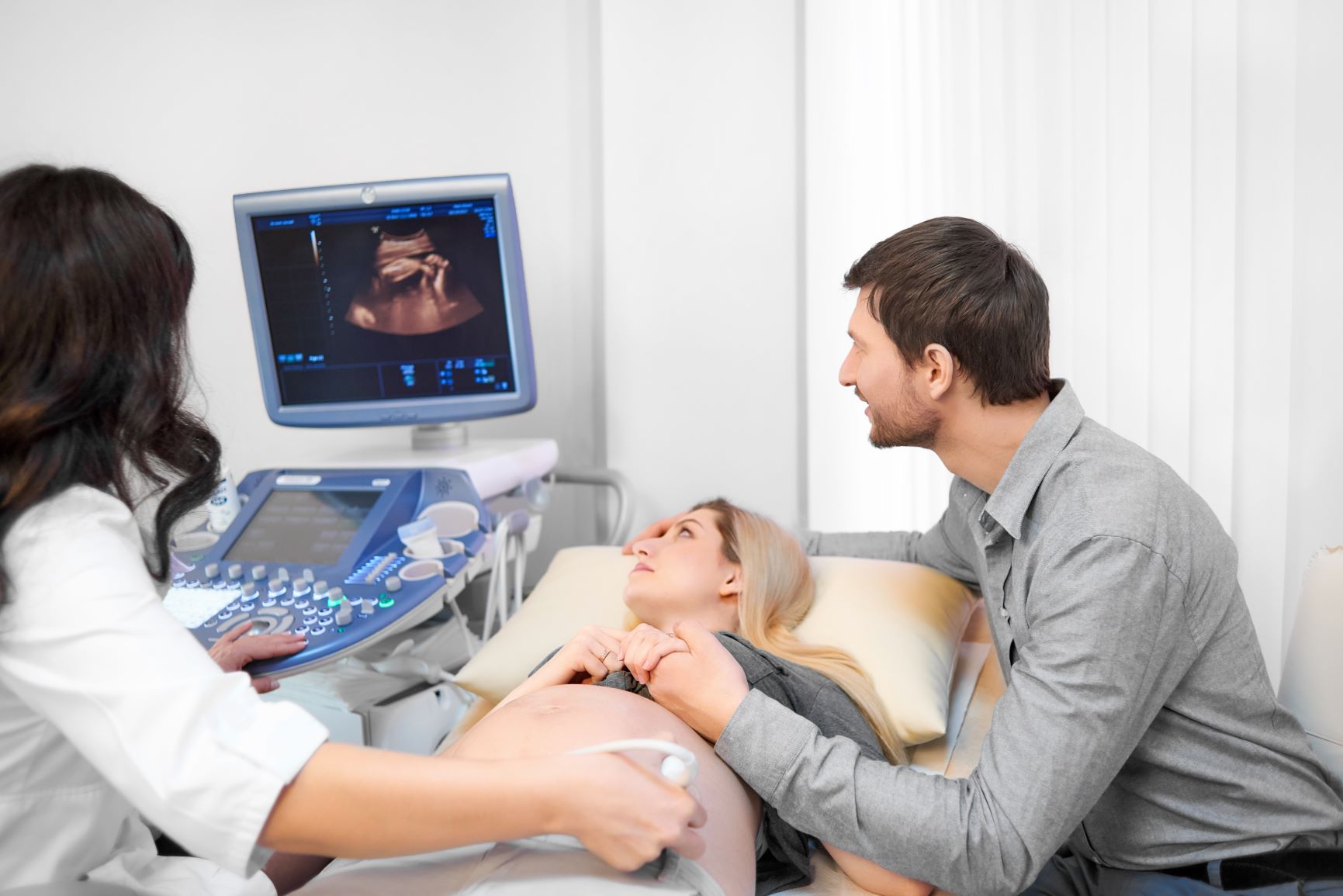
Pregnancy scans
Alongside taking your supplements, eating a balanced diet and engaging in physical activity, you will be able to check the health of you and your developing baby through the routine pregnancy scans offered to all expectant mothers either on the NHS or through private services.
Maternal Mental Health Matters Awareness Week
But one area that is often not discussed and is the hardest to change is your emotional wellbeing. Lucie who is a specialist in mental health during pregnancy and the immediate postnatal period, says that your emotional health is just as important as your physical health. Maternal Mental Health Matters Awareness Week, which takes place between 4th and 10th May is aimed at providing more awareness and information on mental health during pregnancy and reducing the stigma that many mothers encounter.
It is very common for women to experience a decline in mental health during pregnancy and indeed after birth. Mothers may feel anxiety symptoms and low mood. It is important to take note of any significant emotional changes during your pregnancy and after your baby has been born and seek support from your Midwife, GP or obstetrician as early as possible.
Some of the early signs to look out for include feeling more irritable and frustrated; crying or often being on the verge of crying most days; feeling unable to cope; having negative thoughts about yourself and/or your baby; worrying unnecessarily about things that wouldn’t normally bother you; being overly anxious or afraid of being left alone with your baby; or having intrusive images about harming your baby. It is understandably very difficult for expectant and new mothers to talk about such feelings, especially to health professionals, without the fear of being judged.
However, health professionals are always there to listen and support you through your journey into motherhood. It is important that as part of the discussions you have during your pregnancy and after giving birth that you are not afraid of telling your midwife or health visitor how you are feeling. This can help identify whether any further support is required early on.
 It is believed that one in four new mothers will suffer from postnatal depression within the first year following the birth of their baby. The vast majority will only experience mild symptoms, such as feeling sad a lot of the time or having trouble sleeping even when the baby is or sleeping excessive amounts. However, for some new mums, these feelings may develop into a severe depressive illness or other severe mental health problems such as post-partum psychosis, a rare psychiatric illness affecting approximately one in one thousand women, which requires specialist input. It is for this reason that it’s important you speak to a healthcare professional early on if you have had, or believe you may be suffering from, mental health issues during your pregnancy or after the birth of your baby.
It is believed that one in four new mothers will suffer from postnatal depression within the first year following the birth of their baby. The vast majority will only experience mild symptoms, such as feeling sad a lot of the time or having trouble sleeping even when the baby is or sleeping excessive amounts. However, for some new mums, these feelings may develop into a severe depressive illness or other severe mental health problems such as post-partum psychosis, a rare psychiatric illness affecting approximately one in one thousand women, which requires specialist input. It is for this reason that it’s important you speak to a healthcare professional early on if you have had, or believe you may be suffering from, mental health issues during your pregnancy or after the birth of your baby.
Equally important, but something that is often forgotten about, is the support that partners may also need. Whether this is due to sleep deprivation, financial concerns, the additional responsibilities of becoming a parent, the change in family dynamics at home, or the guilt brought on in not being able to breastfeed during the night, your partner can also develop postnatal depression. In fact, the number of partners who become depressed in the first year is double that of the general population. Studies have shown that, like new mothers, one in 10 partners experienced post-natal depression and are more likely to do so if there are maternal mental health issues. Statistics show partners are more likely to suffer from depression three to six months after their baby is born. If you feel your partner could be depressed please encourage them to seek advice and support from their GP.
It is often very difficult to diagnose an individual with depression or other mental health issues because the symptoms, particularly early on, are often confused with the ‘baby blues’ which is something that is experienced by a large percentage of mothers. This is a time when you may feel low and tearful, usually occurring in the few weeks after birth and is often caused by normal hormonal changes taking place in your body. Such feelings will improve with time, but again it is important to speak to your health visitor or GP if you or your partner do not see any improvement.
The good news is that there is a wide range of specialist perinatal support services now available for expectant and new parents. The difficulty is that it may not always be obvious of who to approach or what help to ask for. The important thing is that you are open and honest with the health professionals that are involved during your pregnancy, birth and postnatal care. Making a note of any changes in mood or feelings and describing your symptoms will ensure you get the right care and support for you and your baby. Please remember… A happy mother is a happy baby even during pregnancy.
Year of the Nurse and Midwife
2020 marks the first ever global Year of the Nurse and Midwife. It has been designated as such by the World Health Organisation to celebrate the bicentennial year of Florence Nightingale and provides a fantastic opportunity to highlight the extraordinary work of nurses and midwives across the globe. And this couldn’t be a more momentous year to do so given the extreme pressures the NHS and other health providers across the globe are currently under helping to tackle the global pandemic we face.
Maternity Care









